ACL reconstruction surgery is usually recommended for most active persons with ACL tears. The surgery is performed arthroscopically ("keyhole" surgery with 2 small holes in the front of the knee). The replacement tissue for the ACL is known as the "graft". This graft is tunneled through drill holes made in the tibia (leg bone) and femur (thigh) bone and fixed in the position of the original ACL.
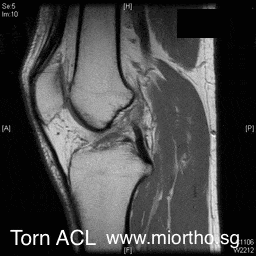
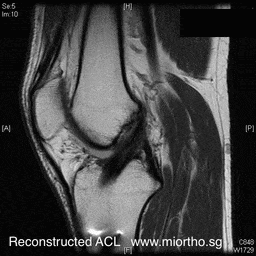
The graft usually taken from:-
- other parts of the patients own body
- hamstring tendon (from the hamstring muscle at the back of the leg, still leaving most of the muscle intact)
- patellar tendon (the middle one-third) of the tendon in front of the knee.
- same tendons as above but opposite leg
- other tendons
- donated tissue, known as allograft
The main tendons used are the patient's own hamstring tendon, or patellar tendon from the same knee as the ACL injury. Each of these two tendons has its own advantages and disadvantages. In the past, the patellar tendon graft was more commonly used for all patients. However, in recent years, the majority of sports surgeons around the world use the hamstring tendon. Opposite leg grafts and allografts are usually reserved for more complex cases, or in revision surgery, where previous ACL reconstruction grafts have ruptured. Allografts are not recommended as the primary graft for most patients; at least one recent research study from the USA has shown that the long term 10 year re-tear risk of allografts was 3 times more than patients who had their own tissues used (25% of patients with allograft had their grafts tear within 10 years after surgery, compared to 8% for patients who had used their own tissues).
ACL reconstruction surgery is usually performed with a 1 night stay in hospital. Some patients chose to do surgery as a day surgery case, while others might need to stay in hospital for 2 nights. After surgery, patients need to use crutches to reduce the weight on the operated leg for about 1-3 weeks, depending on their comfort level, and confidence. Knee braces after surgery are usually not required. Intensive physiotherapy starts almost immediately, and patients would need regular physiotherapy for at least 6 to 9 months, to gain the greatest benefit of the operation.
Typically, many patients start major resistance exercises and stationary bicycle exercises with resistance at about 2 months, and start running at about 5 months. We recommend a gradual introduction of functional exercises and agility exercises from 8-9 months after surgery, with a gradual return to full sports thereafter. After 1 year, the success rate of the surgery in allowing patients to return to their previous level of sporting activity is about 85-90%.
