 Patients who have a history of shoulder dislocation, or have symptoms and clinical signs of shoulder instability, may benefit from shoulder stabilisation surgery. Traditionally the surgery is performed using an open operation with a 5 to 8 cm incision in the front of the shoulder. Over the last 25 years, arthroscopic "keyhole" techniques utilising 3 small 1cm incisions, have become the gold standard for sports surgeons to perform the same operation.
Patients who have a history of shoulder dislocation, or have symptoms and clinical signs of shoulder instability, may benefit from shoulder stabilisation surgery. Traditionally the surgery is performed using an open operation with a 5 to 8 cm incision in the front of the shoulder. Over the last 25 years, arthroscopic "keyhole" techniques utilising 3 small 1cm incisions, have become the gold standard for sports surgeons to perform the same operation.
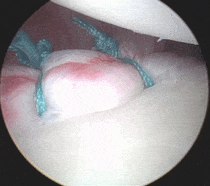
Arthroscopic shoulder stabilisation involves placing small bioabsorbable (non-metallic) anchors into the bone of the glenoid (socket). These anchors have sutures attached to them, and it is these sutures that are used to stitch the Bankart/labrum tear back into place. The surgery can be performed as a day surgery operation. Waterproof dressings are applied, so that patients can shower normally on the evening after surgery. Patients usually need to wear a sling (to allow the repaired labrum to heal back to the bone) for about 4 weeks. Physiotherapy starts almost immediately. Most patients recover fully by 4-6 months. In most patients, the risk of repeat dislocation is estimated to be less than 5-10%.
Some patients, especially those with many previous repeat dislocations, may have damage to the glenoid or "cup side" of the shoulder. If there is a loss of more than 20% of the width of the glenoid cup, arthrosocpic labral repair may have a higher chance of failure. This is also true in younger patients, and patients participating in contact sports like rugby.
In this difficult group of patients, arthroscopic labral techniques may have a failure (re-dislocation) risk of more than 30-40%. For these patients, an operation to transfer a piece of bone from the front of the shoulder to the glenoid to act as a "bony bumper" may be needed. This is the so-called "Latarjet procedure", and may be needed in patients who have had a failed arthrosocpic labral surgery, have bony glenoid damage, or younger patients planning to return to contact sports.
